AI could predict patients’ future health conditions, study finds | Science & Tech News

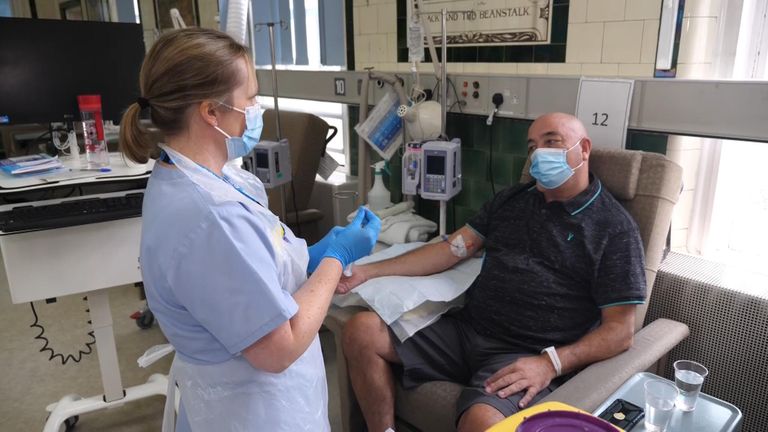
Artificial intelligence (AI) could be used to predict the type of health conditions a patient is likely to develop in the future, a study has found.
The technology could be used to help doctors when it comes to monitoring patients or making decisions around diagnosis, researchers said.
The AI tool, known as Foresight, belongs to the same family of AI models as ChatGPT but has been trained using information from NHS electronic records.
It was developed by researchers from King’s College London (KCL), University College London (UCL), King’s College Hospital NHS Foundation Trust and Guy’s and St Thomas’ NHS Foundation Trust.
The researchers trained three different models of Foresight using data from more than 811,000 patients from two NHS trusts in London and a publicly available dataset in the US.
It was given 10 possible disorders a patient may experience next based on their records.
When using data from NHS hospitals, Foresight was able to correctly identify the condition 68% and 76% of the time. It was accurate 88% of the time when using US data.
Read more on Sky News:
Alcohol-free beer on draught ‘could improve public health’
Mother of missing British woman asks Biden for help finding her daughter
Zeljko Kraljevic, research fellow in health informatics, biostatistics and health informatics at KCL and the first author of the study – published in The Lancet Digital Health – said the findings show the tool “can achieve high levels of precision in predicting health trajectories of patients, demonstrating it could be a valuable tool to aid decision-making and inform clinical research”.
Senior author Richard Dobson, a professor of medical informatics at KCL and UCL and theme lead for informatics at the National Institute for Health and Care Research (NIHR) Maudsley Biomedical Research Centre (BRC), said: “It is an exciting time for AI in healthcare, and to develop effective tools we must ensure that we use appropriate data to train our models and work towards a shared purpose of supporting healthcare systems to support patients.”
The research team is now seeking more hospitals to be involved in developing Foresight 2, which Prof Dobson said will be “a more accurate language model”.