First child to get new cancer treatment among 100,000 given early access to drugs in NHS milestone | UK News
Nearly 100,000 cancer patients have now had fast-track access to newly approved NHS drugs – with one teen saying his treatment felt like being on a “slope going up”.
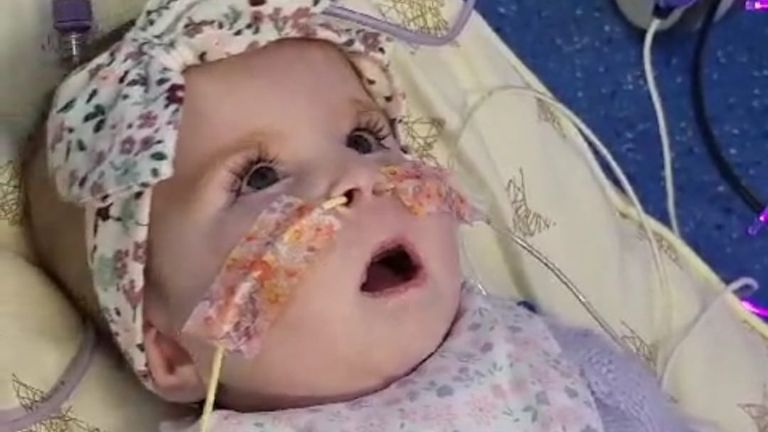
Yuvan Thakkar, 16, was the first NHS patient to receive a therapy that uses the body’s own cells to fight cancer.
He was diagnosed with a form of leukaemia aged six and received the pioneering treatment at Great Ormand Street Hospital.
The CAR-T therapy, called tisagenlecleucel (Kymriah), involved removing his immune cells and modifying them to recognise and destroy cancer cells, before reintroducing them to the body.
In April, the NHS will have helped 100,000 patients access new and innovative treatments over eight years.
It’s been made possible by the NHS Cancer Drugs Fund – set up in 2016 to give patients faster access to new treatments.
The fund benefits people with common cancers, such as breast, lung, colorectal and prostate; as well as those with less common ones such as ovarian, cervical, kidney, and leukaemia – and also rare cancers including thyroid and biliary tract.
NHS England said patients get access to National Institute for Health and Care Excellence (NICE) approved treatments six months faster, and all cancer treatments are funded as soon as they are approved.
For Yuvan, who spent his childhood in hospital fighting leukaemia, faster access to the CAR-T therapy means he is now able to sit his GCSEs.
Recounting his treatment, he said: “I remember receiving the cells for a bit. I was feeling quite down” – before being sent to intensive care “where I couldn’t do basic counting and things like that”.
The teenager said he doesn’t remember any of his treatment until it was finished.
“I thought I could start to get better, then I remembered, ‘oh, I can do this, I can do that’. And from now on, it’s just been like a slope going up,” said Yuvan.
Concern as cancer targets cut
Professor Sir Stephen Powis, the NHS England medical director, said treating 100,000 people was “a fantastic milestone”.
He said: “This vital fund is helping ensure patients get access to the most promising drugs far quicker than would otherwise be the case, helping people with cancer like Yuvan receive a life-changing intervention that sets a path for a longer, healthier life spent with family and friends”.
However, Professor Pat Price, a leading oncologist and co-founder of the Catch Up With Cancer campaign, is concerned about those still struggling to get treatment due to the backlog of cancer cases.
Read more from Sky News:
Contraceptive injections linked to brain tumour risk
Preventative therapies ‘can cause cancer to hibernate and return’
Since the pandemic, she said 250,000 patients have not had their treatment on time.
National guidance states 85% of people should begin treatment within two months, or 62 days, of an urgent referral, but Professor Price said there has been a downgrade in ambition.
She told Sky News: “We are in the biggest cancer crisis we’ve ever had. This week the NHS have reset their targets for 2025 and sadly, they’ve pushed their recovery target for cancer.”
She said the target for next year had been cut from 85% to 70%.